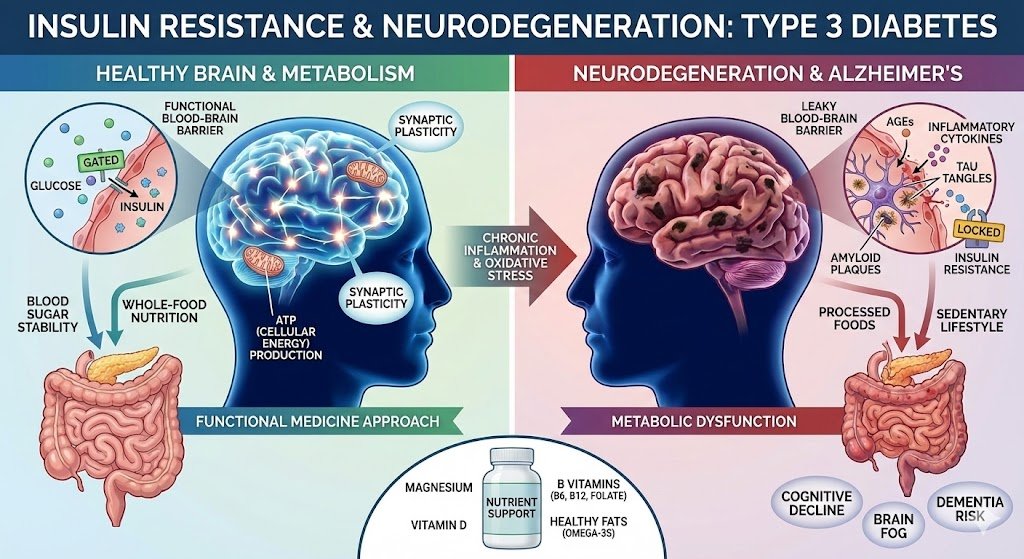
For decades, insulin was viewed as a hormone that only mattered for blood sugar. Functional medicine understands that insulin is also a critical brain hormone, essential for memory, cognition, and neuronal survival. When insulin signaling breaks down, the brain quite literally begins to starve.
This breakdown helps explain why Alzheimer’s disease is increasingly referred to as “Type 3 Diabetes.”
1. Root Cause Explanation: Insulin Resistance Starts Long Before Memory Loss
Insulin resistance is not just a blood sugar problem — it is a cellular energy crisis.
What insulin normally does
- Transports glucose into cells so it can be converted into ATP (energy)
- Supports neurotransmitter signaling
- Protects neurons from oxidative damage
- Regulates learning, memory, and synaptic plasticity
What happens with insulin resistance
- Cells stop responding properly to insulin
- The pancreas produces more insulin to compensate
- Over time, insulin signaling becomes impaired system-wide — including in the brain
Key functional insight:
Abnormal glucose metabolism can begin 20–30 years before Type 2 diabetes is diagnosed. Neurodegeneration often follows decades later.
2. The Three Types of Diabetes (Functional Medicine Perspective)
Type 1 Diabetes
- Autoimmune destruction of pancreatic beta cells
- Little to no insulin production
- Requires lifelong insulin therapy
Type 2 Diabetes
- Insulin is present, but cells are resistant
- Blood glucose remains elevated
- Often driven by diet, inflammation, stress, and toxins
Type 3 Diabetes (Neurodegenerative Insulin Resistance)
- Insulin resistance localized to the brain
- Impaired glucose uptake by neurons
- Strongly associated with Alzheimer’s disease
This explains why not all diabetics develop Alzheimer’s, but diabetes significantly raises the risk.
3. Why the Brain Is Especially Vulnerable
The brain uses 20–25% of the body’s total glucose, despite being only ~2% of body weight.
In Alzheimer’s disease:
- Brain insulin levels are significantly reduced
- Insulin receptors on neurons decline early in the disease
- Neurons cannot efficiently use glucose
- Energy production drops → neurons starve → degeneration and cell death occur
This leads to:
- Loss of brain volume
- Cognitive decline
- Memory impairment
- Increased vulnerability to oxidative stress
4. System Connections: Blood Sugar, the Blood–Brain Barrier, and Amyloid Plaques
The Blood–Brain Barrier Problem
In insulin resistance:
- Glucose continues to cross the blood–brain barrier
- Insulin transport into the brain is impaired
- Result: high glucose, low insulin inside the brain
The Amyloid Connection
Excess glucose reacts with proteins and fats, forming:
- Advanced glycation end products (AGEs)
- Amyloid-beta peptides
- Amyloid plaques — a hallmark of Alzheimer’s disease
This creates a vicious cycle:
- High glucose → oxidative stress → inflammation → more insulin resistance
5. The Role of Dietary Sugars (Not All Sugars Act the Same)
Glucose
- Rapidly absorbed
- Directly raises blood sugar
- Requires insulin for cellular entry
Fructose & Galactose
- Processed first by the liver
- Converted into glucose
- Slower blood sugar rise — but harmful in excess
- Contributes to insulin resistance and fatty liver
Functional takeaway:
Chronic overconsumption of sugar — especially refined carbohydrates — drives insulin resistance years before disease appears.
6. Why Drugs Alone Don’t Fix the Problem
Some diabetic medications (e.g., insulin sensitizers like rosiglitazone):
- Temporarily improve insulin sensitivity
- Do not correct underlying metabolic dysfunction
- Comes with significant side effects
Even promising therapies like intranasal insulin (which bypasses the blood–brain barrier and has shown improvements in early Alzheimer’s) highlight the same truth:
The issue is not insulin deficiency alone — it is insulin signaling dysfunction.
7. Additional Root Contributors to Neurodegeneration
Insulin resistance is a major driver — but it is not the only one.
Functional medicine recognizes multiple overlapping contributors:
- Chronic inflammation
- Oxidative stress and free radical damage
- Accumulation of AGEs
- Poor diet quality
- Chronic psychological stress
- Environmental toxins
- Heavy metals
- Physical trauma and brain injury
- Mitochondrial dysfunction
- Nutrient deficiencies like Vitamin D, B6, B12, Folate and Magnesium
This explains why some individuals with diabetes never develop Alzheimer’s, while others do.
8. Functional Medicine Solutions: Addressing the Root Cause
True prevention and intervention require systems-based healing, not symptom suppression.
Key strategies include:
- Blood sugar stabilization through whole-food nutrition
- Reducing dietary sugar and ultra-processed foods
- Supporting mitochondrial function
- Reducing inflammation and oxidative stress
- Improving insulin sensitivity through lifestyle interventions
- Addressing gut health, toxins, and nutrient deficiencies
- Movement, sleep, and stress regulation
9. Call to Action: Protect Your Brain by Protecting Your Metabolism
Alzheimer’s disease does not start in the brain — it starts in metabolic dysfunction years earlier.
If you are dealing with:
- Blood sugar instability
- Prediabetes or diabetes
- Cognitive changes
- Brain fog or memory decline
- Family history of Alzheimer’s
👉 Now is the time to intervene — not wait.
Functional medicine empowers us to identify dysfunction early, correct root causes, and protect long-term brain health.
PubMed References
- Elizabeth M. Rhea, Manon Leclerc, Hussein N. Yassine, Ana W. Capuano, et al. (2023) — State of the Science on Brain Insulin Resistance and Cognitive Decline Due to Alzheimer’s Disease. DOI: 10.14336/AD.2023.0814
- C.L. Lanzillotta, et al. (2024) — Bridging brain insulin resistance to Alzheimer’s pathogenesis. DOI: 10.1016/j.tibs.2024.09.004
- G.E. Ennis, T.J. Betthauser, R.L. Koscik, et al. (2023) — The relationship of insulin resistance and diabetes to tau PET SUVR in middle-aged to older adults. DOI: 10.1186/s13195-023-01180-2
- Wenqiang Chen, PhD, Ronald Kahn, MD, and colleagues (2025) — Insulin’s role in brain health and link between diabetes and Alzheimer’s disease. DOI: 10.1073/pnas.2501527122